Vein Center
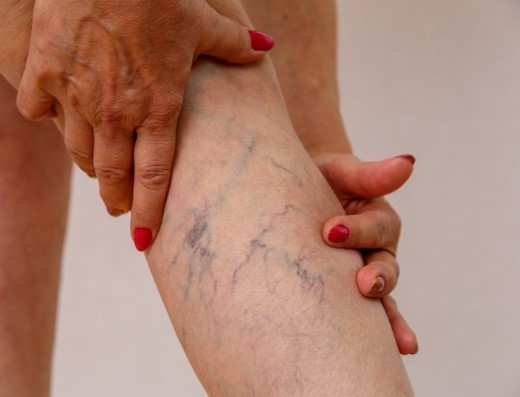
Did you know that 40% of women and 25% of men suffer from the physical and/or social discomfort of varicose veins, or that 1 out of 2 people over the age of 50 report having this condition? Thanks to emerging technology and advanced techniques, Highpoint Health Vein Center offers the highest level of patient care and best possible outcomes with fewer complications and less recovery time.
Take a Peripheral Artery Disease Assessment
If you have questions about peripheral artery disease, start with a health assessment and learn more about any risks you may have for this condition.
Next Steps
Find a Doctor
Take a Health Risk Assessment
Venous Insufficiency
Over 40 million Americans suffer daily with painful, swollen legs as a result of venous disease. This condition is the result of faulty valves in the veins and is called venous insufficiency. In a healthy vein, there are one-way valves that allow the blood to move toward the heart, but not away. In a diseased vein, these valves do not work properly, allowing the blood to fall downward in between heartbeats. This back and forth motion of blood leads to an increased venous blood pressure resulting in inflammation of the tissues around the vein. This inflammation can cause leg pain, swelling, bulging varicose veins, heaviness, restlessness, cramps, skin discoloration, numbness, tingling, ulcers, blood clots, and deep venous thrombosis (DVT). Left untreated, this condition only worsens over time.
Risk Factors
Heredity is the number one risk factor for venous disease. If your parents had varicose veins, you have an 89% chance of developing them. Next to heredity is gender. Women, especially those that have had multiple pregnancies, are three times more likely than men to develop venous disorders. Additionally, professions that require long periods of sitting or standing, increase one’s risk for venous disease. Age is also a risk factor. While older people are at a higher risk for venous disease, it can start as early as childhood.
Treatment
The treatment for this disorder is called radiofrequency ablation. This is a minimally invasive procedure where a catheter is inserted into the diseased vein by way of a small (2-3 mm) incision. Heat is applied to the vein walls causing it to close. Your body then naturally re-routes the blood through other healthy veins. The procedure is done under local anesthetic and is covered by most insurance carriers, including Medicare. Patients walk out of the Vein Center and return to their normal activities the same day.
Treatment may also include chemical vein ablation, another minimally invasive procedure that involves injecting a foam into the veins, causing them to close. This procedure does not require incisions or stitches.
Spider Veins
Spider veins are a result of dilated venous capillaries that fill with blood and become visible. These are not considered harmful and are often treated for cosmetic reasons. Sclerotherapy involves injecting a solution into the spider vein, which causes the vein wall to seal shut, therefore stopping the blood flow. The vein will turn to scar tissue and fade away over a period of weeks.
